On a chilly morning in Hawkins County, Sam McMurry stands in the middle of a brightly lit conference room watching as wall-mounted monitors light up with red blips. There’s about a dozen of them total, all overlaid on a map of the county.
They indicate emergency calls, anything from breathing problems to a car crash. It’ll take only a few minutes for any one of the county’s six ambulances to reach them. But from there, most patients are in for at least a 30 minute ride to the nearest hospital. For others, it might take an hour. Those long rides in a medical crisis mean odds are not always in people’s favor.
McMurry is a sergeant with the Hawkins County Emergency Medical Service, a non-profit team of EMTs and paramedics who are responsible for administering intravenous care and getting patients to hospitals during emergencies.
 “Everyone thinks that we show up, you’re going to the hospital,” McMurry said. “But there’s other ways we can help.”
“Everyone thinks that we show up, you’re going to the hospital,” McMurry said. “But there’s other ways we can help.”
One of those ways, McMurry believes, is to treat sepsis patients before the ambulance delivers them to a hospital. His theory came after a couple of years observing a trend with those red blips on the EMS map.
A lot of them were people complaining of general, severe pain all over.
Ambulance crews frequently treated those calls like a heart attack. They’d give patients drugs to help their blood pressure or ease their pain, but couldn’t adequately diagnose the problem for themselves. Some were worse by the time they made it to the nearest hospital.
It was there that doctors found the problem: these patients had out-of-control infections that had become septic. In some cases it was too late to save them.
“The surge of patients that we’ve gotten when we was looking into sepsis was just unbelievable,” McMurry said. “Why are we not doing more to help these patients in these situations?”
More in this series: Healthcare Hollow
When there’s no easy access to a hospital in rural areas, the number of deaths from sepsis is higher, according to the National Institutes of Health. That’s a real challenge in Hawkins County, a sprawling rural area with just one five-bed hospital and no interstate access. If someone is having an emergency – like sepsis – the geography and distance can be risky.
That’s why the county’s EMS agency is partnering with the region’s hospital operator, Ballad Health, to make antibiotic treatment available on ambulances for the first time. For decades, paramedics and EMTs were taught to treat symptoms instead of underlying problems.
‘It got really bad, really fast’
If an infection is left untreated, people enter a state of shock known as sepsis where their body begins to attack itself. It’s a severe, life-threatening condition. According to the Centers for Disease Control and Prevention, it affects nearly 2 million adults in the U.S. every year. About 20% of them will die from it.
McMurry has seen firsthand how dangerous sepsis can be in his own family. Last October, his wife, Brianna, went to the hospital to give birth to their daughter. There hadn’t been any complications, and she came home from the hospital after a few days.
It had been a 45-minute car ride home, and she was ready to lay down and rest. That’s when the pain began.
“I started having pain in my upper abdomen,” Brianna said. “We couldn’t get it to calm down.”
She said she couldn’t get comfortable, and she was sick to her stomach. She thought it might have been her gall bladder. So they turned around and went back to the hospital – another 45-minute drive. All the while, Brianna was getting worse.
“It got really bad, really fast,” she said.
 As it turns out, she had developed an infection while giving birth. It had gone unnoticed and become septic. Luckily, she made it back to the hospital in time to receive life-saving antibiotics. But many others in Hawkins County aren’t so lucky.
As it turns out, she had developed an infection while giving birth. It had gone unnoticed and become septic. Luckily, she made it back to the hospital in time to receive life-saving antibiotics. But many others in Hawkins County aren’t so lucky.
His wife’s experience with sepsis reinforced what Sam already knew: Sepsis is one of the leading causes of hospitalization in Hawkins County. At one point, about 20% of the calls Hawkins County EMS received were for sepsis. Something had to change.
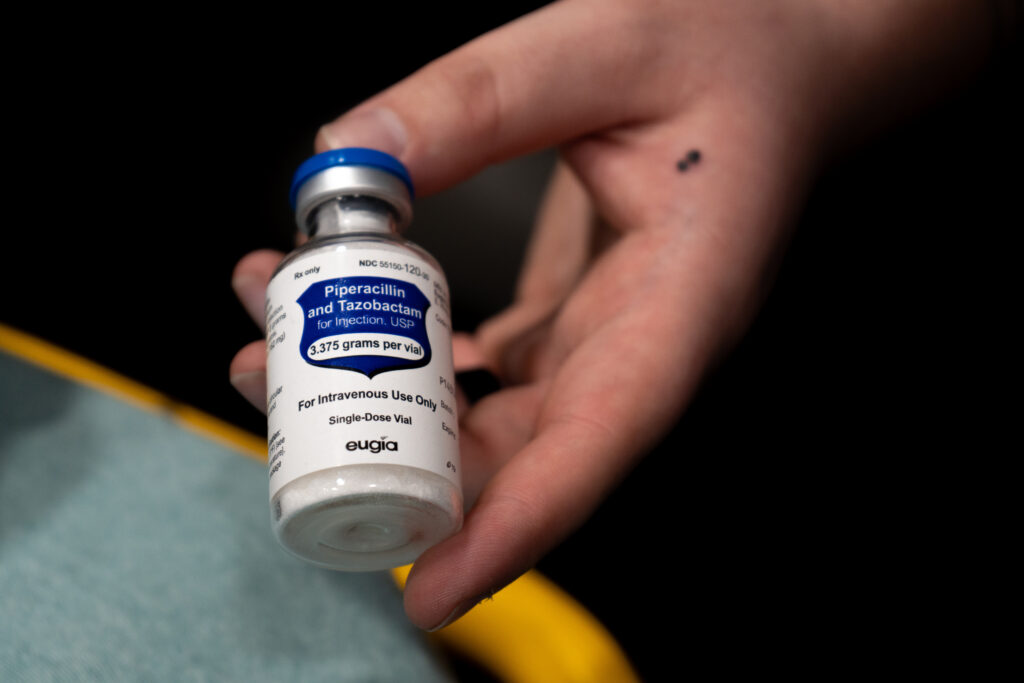
“That’s where the antibiotic administration comes in,” McMurry said. “We’re directly attacking the problem that’s causing the body to attack itself.”
‘I was so excited’
Around July of last year, Hawkins County EMS began equipping ambulances with antibiotics for the first time. They hoped their paramedics and EMTs would be able to identify and treat septic patients all before they reached the emergency room.
Paramedic Jacob Adams says it was a game changer.
“I was so excited to try it,” Adams said. “I’ve been a fan of it since we first got it. If there’s anything we can do that could potentially produce better outcomes for patients, I think it’s completely worth it.”
This type of protocol is harder to adopt in a more urban area where there might be as many as three or four different hospital operators. EMS agencies have to clear their treatments with each one, which can be complicated.
That’s not the case with Ballad Health, a state-sanctioned monopoly which operates 12 hospitals across eight East Tennessee counties. Since they have the approval from Ballad, septic patients in Hawkins County can be checked for sepsis the moment they get in the ambulance and receive antibiotics right away.
And the program is already showing signs of positive results. Dr. Lauren Py is the Medical Director of Holston Valley Medical Center in Kingsport. She says clinical conditions are improving for septic patients arriving from Hawkins County.
“We’re identifying these patients sooner,” Py said. “They might pick them up and they were hypotensive. They’ve already gotten their fluids, they’ve gotten antibiotics, and by the time they come to the ER, maybe they’re talking more and they’re more alert. So I mean, clinically, you can see improvement.”
 But nothing can be proven for sure yet, according to Knoxville-based ER Doctor Todd Heffern. He’s the medical director for Hawkins County EMS, and says they need much more data before their approach can be formally declared a success.
But nothing can be proven for sure yet, according to Knoxville-based ER Doctor Todd Heffern. He’s the medical director for Hawkins County EMS, and says they need much more data before their approach can be formally declared a success.
“I don’t think you’re ever going to get the volume here,” Heffern said. “Sepsis studies – where we really base our treatments on – are tens, if not hundreds-of-thousands, of patients.”
Hawkins County sees less than 10 septic patients every month. That’s why he’s hoping other counties in Tennessee – and the U.S. – will adopt similar programs.
This story is part of our Healthcare Hollow series, made possible, in part, by the NIHCM Foundation.

