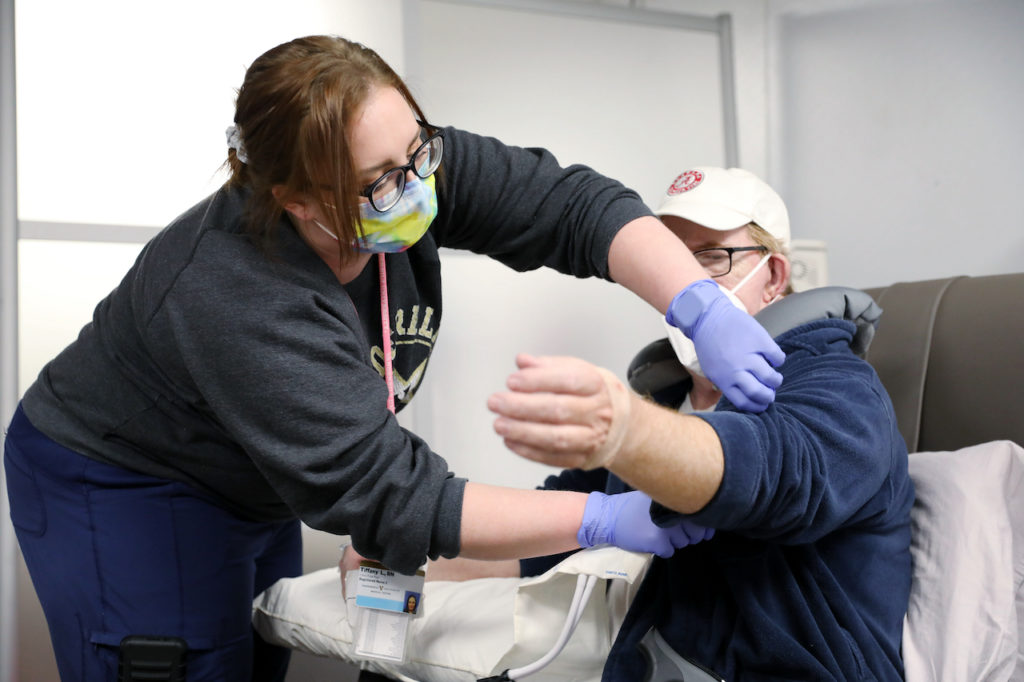
Vanderbilt University Medical Center credits an experimental COVID-19 treatment with keeping dozens of patients out of the hospital in recent weeks. It’s the same infusion that President Trump credits with his quick recovery from the virus.
Hospitals have been slow to embrace monoclonal antibodies, even though the injections developed by Eli Lilly are paid for by the federal government, because the logistics are such a pain. Patients have to be treated early on and their disease has to be mild even though they’re at high risk of complications.
Also, it requires a dedicated site, because COVID-positive patients can’t be sitting next to everyone else, like in a chemotherapy infusion center. So Vanderbilt used part of its parking garage, and it looks kind of sketchy, says Nora Gilgallon-Keele. She works at the medical center but had trouble finding it.
“It’s a little frightening, honestly, if you didn’t know what it was,” she says. “Let’s just go into this fenced-in, construction-looking area and get hooked up to an IV and get we don’t know what.”
In November, the FDA began allowing its use on an emergency basis, but only for seniors or high-risk patients like Gilgallon-Keele. She has a weakened immune system from medication she takes.
Just after Christmas, when she started getting achy and weak, she tested positive for COVID. Vanderbilt reached out to see if she wanted to try the antibody infusion.
“All I could think of is, I did not want to end up in the hospital. I did not want to end up on a respirator,” she says. “I did not want to end up dying.”
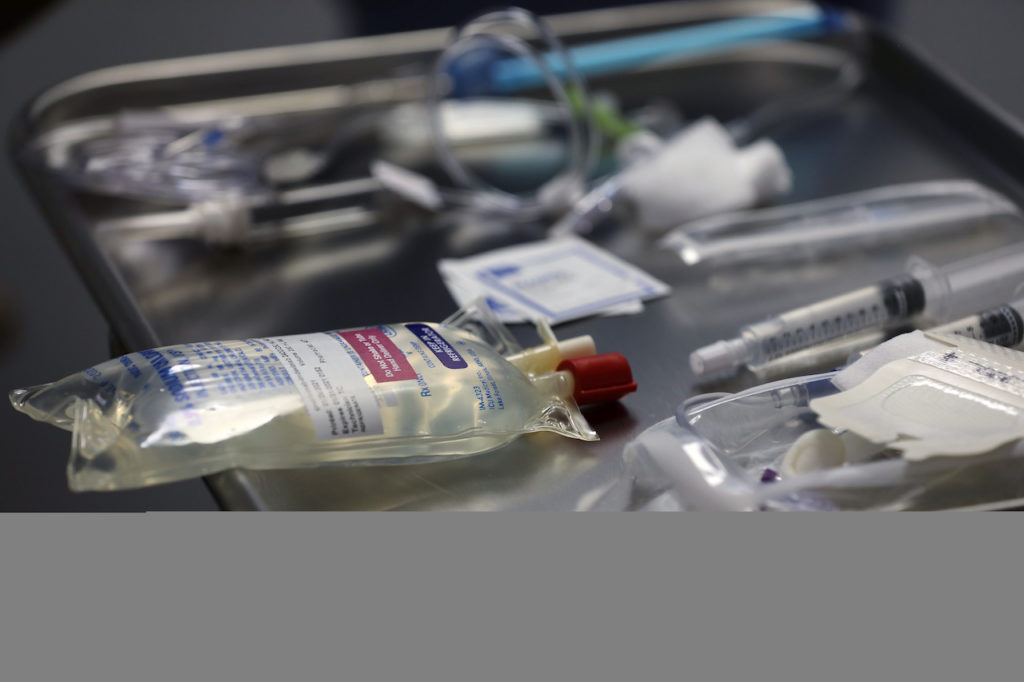 Erin O. Smith Vanderbilt University Medical Center
Erin O. Smith Vanderbilt University Medical CenterPatients receive an infusion within 10 days of symptoms first showing up. Pharmaceutical companies Eli Lilly and Regeneron have both developed monoclonal antibody treatments for COVID-19. Vanderbilt University Medical Center also has its own antibody treatment developed with AstraZeneca that is in the final phase of clinical trials.
Reducing hospitalizations
So she accepted the risk of taking a relatively unknown drug. Within a few hours, she was at the makeshift infusion center.
The 60-year-old program manager didn’t get better right away, but she says she didn’t get any worse — nowhere near needing a hospital. And that’s exactly the point.
“Its benefit is really in keeping people out of the hospital,” says Dr. Patty Wright, an infectious disease specialist who oversees the monoclonal antibody program at Vanderbilt.
The medical center has given the antibody treatment to nearly 1,000 patients. Only about 4% have been hospitalized — roughly half of what’s expected without treatment.
“Which has been huge on these days when we’ve been so incredibly full of patients,” she says. “To keep 40 or 50 patients out of the hospital is amazing.”
The makeshift infusion center is now operating seven days a week.
There are still many in the medical community who are skeptical, since the only studies that have been completed were small. So it’s less clear whether the treatment helped or people got better on their own.
In some parts of the country, major health systems are infusing COVID patients by the thousands. Houston Methodist has treated 2,300. Mayo Clinic has infused 3,500 across three states, with one of its doctors citing just 3% hospitalization. Yet in Spokane, Washington, it’s hard to find the antibodies.
Vanderbilt is impressed enough that Dr. Alex Jahangir, who is a VUMC surgeon and also chairs Nashville’s coronavirus task force, is now adding it to the checklist — wear a mask, get a test, and if sick, consider an infusion.
“If you test positive, ask about monoclonal antibodies,” he said at the city’s weekly briefing on Thursday. “It literally may save your life.”
